Naloxone
What is Naloxone?
- Naloxone (pronounced na-LOX-own) is a prescription medication used to temporarily reverse the effects of opioid drugs (for example heroin, morphine, codeine, methadone, nitazenes and fentanyl) if someone experiences an overdose.
- Naloxone can help to keep a person alive until an ambulance arrives.
- Naloxone works by displacing opioid molecules from their receptors in the body and brain.
There are two types of Naloxone available in Ireland
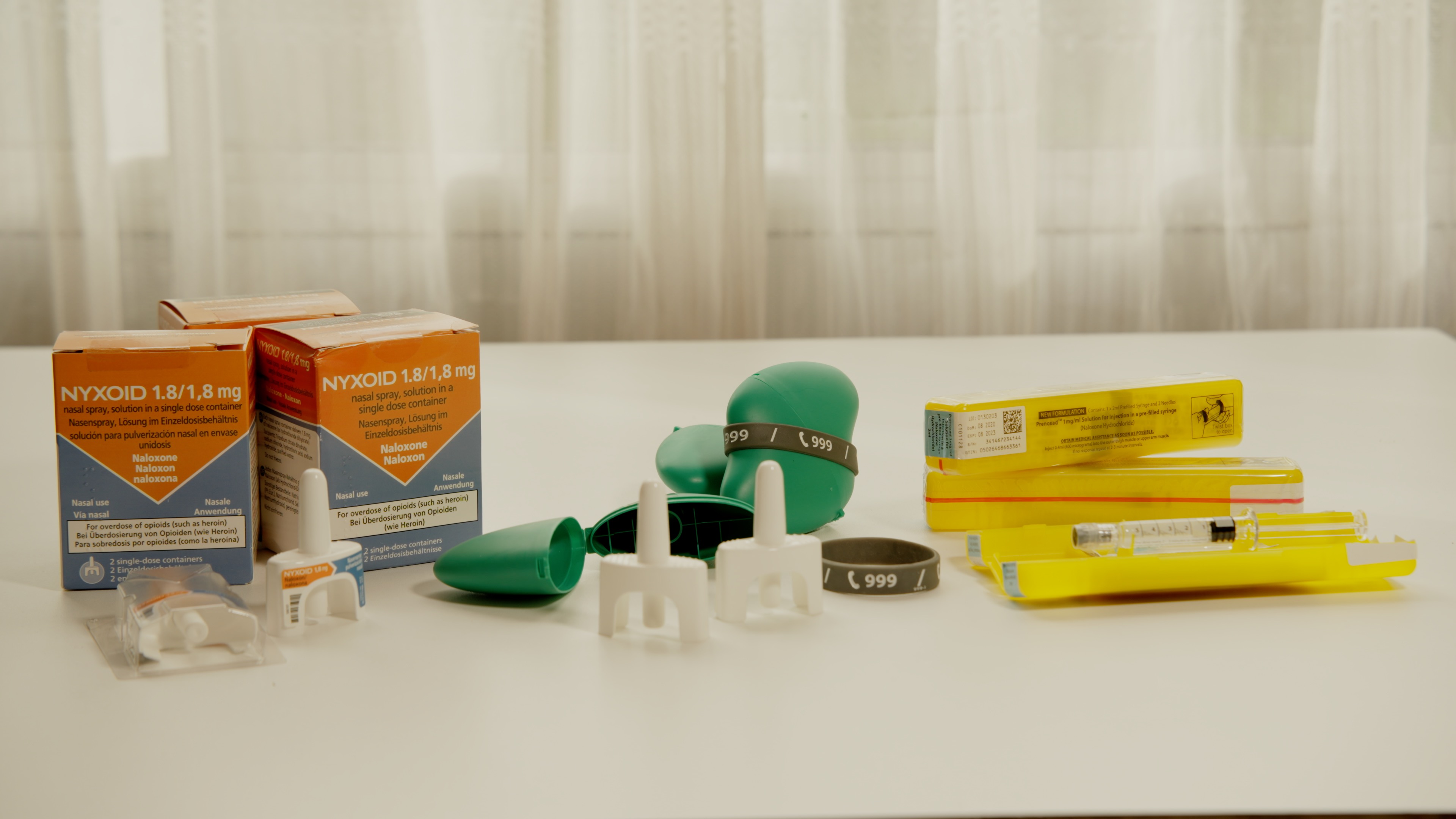
Intramuscular Naloxone (brand name Prenoxad™)
- A pre-filled syringe and needle which once assembled is injected into the middle outer thigh
- Each pack is for SINGLE INDIVIDUAL USE only
- 5 doses of 0.4mg per dose
Intranasal Naloxone (brand names Nyxoid™ and Ventizolve™)
- A needle-free device that requires no assembly
- Each pack contains 2 nasal sprays
- If both doses are required they are sprayed into alternate nostrils
- Each nasal spray is for SINGLE INDIVIDUAL USE only
- Nyxoid™ 1.8mg per dose
- Ventizolve™ 1.26mg per dose
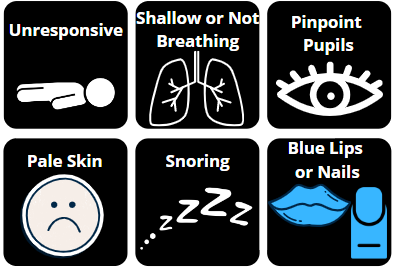
Signs of an opioid overdose
Naloxone and Covid-19
- Please be advised to follow the latest HSE infection prevention and control guidelines regarding the use of appropriate personal protective equipment (PPE) at the time of supporting someone experiencing overdose remains an important mitigation.
From the 1st of June 2023 if the person is not breathing and the person responding is comfortable providing rescue breaths the CPR response can revert to pre-covid guidelines of administering chest compressions and rescue breaths. Responders can continue to provide compression-only CPR after the 1st of June 2023 where they consider there to be a risk, or they are not comfortable providing rescue breaths.
How to respond to an opioid overdose
- If someone is showing signs of an overdose call 112 or 999 for an ambulance without delay
- Check if they are breathing
- If they are NOT breathing start CPR
- If they are breathing put them into the recovery position
- Administer Naloxone and continue CPR (if the person is NOT breathing)
- Administer further doses of naloxone as required
- Wait with them until the ambulance arrives
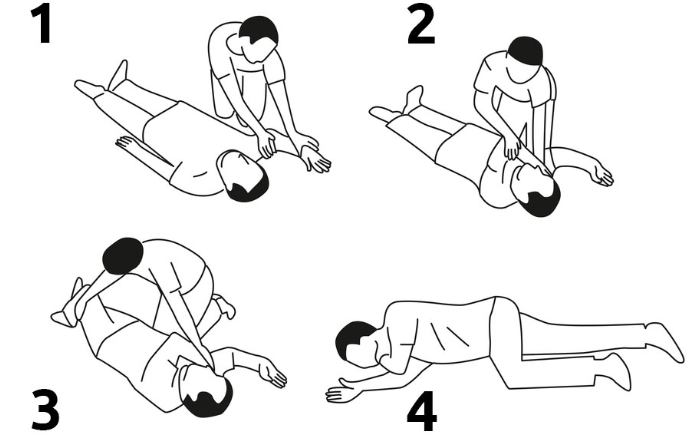
How to move a person into the recovery position
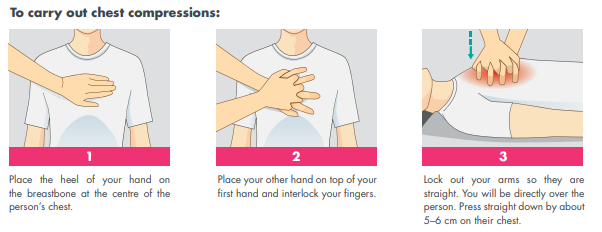
How to carry out chest compressions
Naloxone Training
The Opioid Overdose Awareness and Naloxone Administration Training course, Module 1 is available on HSeLanD. You can find the module by using the “search a module” tool with the key word “naloxone”. This course is open to all HSeLanD users and designed for all frontline workers (clinical and non-clinical) and volunteers who may witness an opioid overdose.
The E-Learning course on HSeLanD is Module 1 of a two module course. It is a pre-requisite, along with current in date CPR training for attendance at the in-person Module 2 training. Successful completion of Module 2 is required for an Organisation to notify the HPRA (via the Emergency Medicines Portal) of its intention to procure or purchase a naloxone from a pharmacy or other supplier for supply and administration in an emergency situation..
Further Naloxone Resources
Download a Step by Step guide How to administer Naloxone here
Download an overdose rescue plan template to use as part of interventions with people at risk here
Video Resources
Get video resources on our site here
Further Information
- Download Frequently Asked Questions (FAQs)
- Download training resources flash cards